Revision Rhinoplasty Surgery in Sydney
All cosmetic surgery involves risks and individual results vary. Cosmetic surgery is a serious decision. Decisions about whether to proceed should be made after careful consideration and following at least two consultations with a qualified medical practitioner.
Revision rhinoplasty — surgery performed on a nose that has already undergone a previous rhinoplasty — is among the most technically demanding procedures in facial surgery. It is also, for many patients, one of the most emotionally significant. The pathway that leads a person to seek revision is rarely straightforward, and the experience of living with an unsatisfactory rhinoplasty result can have a profound impact on wellbeing, confidence, and day-to-day life in ways that deserve to be understood and taken seriously.
This page covers both the surgical and the human dimensions of revision rhinoplasty — the technical complexity, the cartilage grafting, the timing — but also the stress, the psychological weight, and what patients can realistically expect from the process of seeking a second opinion and proceeding with further surgery.
All surgery carries risks — read the full rhinoplasty risks page →
The Emotional Experience of an Unsatisfactory Rhinoplasty
For most people, the decision to have rhinoplasty is not made lightly. It follows months or years of thought, research, and often considerable personal significance attached to the nose — whether because of how it looks, how it functions, or both. Patients arrive at their surgeon’s door with a degree of hope and trust that is rarely extended to any other kind of appointment. When the result does not meet those hopes, the psychological impact can be substantial.
It is important to acknowledge this openly, because it shapes everything that follows: how long a person waits before seeking help, how they describe their concerns at consultation, how they respond to advice about timing, and how they approach the decision whether to proceed with further surgery. Surgeons who work regularly with revision rhinoplasty patients understand that the clinical conversation is never just about cartilage and technique. It is also about trust, grief, and the difficult task of recalibrating expectations.
Grief Over the Original Result
Many patients describe a genuine sense of grief after a rhinoplasty that did not go as they had hoped. This is not an exaggeration or an overreaction — it reflects the fact that the nose is intimately connected with identity and self-image in a way that few other body parts are. A face is how a person presents to the world, and the nose sits at its centre. When that changes in a way that feels wrong, it can feel like a loss of something that was part of who you were.
This grief can take different forms. Some patients feel primarily disappointed — the result was not what they envisioned, but they can put it in perspective and proceed rationally. Others find that their concerns occupy an outsized amount of their mental bandwidth: checking the nose repeatedly in mirrors, photographing it from different angles, avoiding social situations, withdrawing from activities they previously enjoyed. Where concerns are significantly interfering with daily life or causing distress that feels disproportionate, it is worth speaking with a GP or mental health professional in addition to pursuing surgical assessment — not because the concerns are unfounded, but because the distress itself deserves care independently of what surgery can offer.
The Breakdown of Trust With the Original Surgeon
One of the most emotionally complex aspects of an unsatisfactory rhinoplasty is the impact on the relationship with the original surgeon. In most cases, the surgeon did not intend a poor outcome — rhinoplasty is genuinely difficult, healing is unpredictable, and even technically well-executed surgery can produce results that disappoint. But the patient-surgeon relationship in cosmetic surgery involves a particular kind of trust, and when the result falls short of what was discussed and hoped for, that trust is often damaged.
Where the relationship with the original surgeon is still intact and communication remains open, returning to them to discuss concerns is usually the right first step. A surgeon who knows exactly what was done — and why — is better placed than anyone else to assess what has occurred and what options exist. Most reputable surgeons are willing to review their patients honestly, discuss whether further surgery is appropriate, and if so, what it would involve.
Sometimes, however, the relationship is broken. The patient may feel that their concerns were dismissed, that communication broke down, that they were not listened to. In these situations, seeking a second opinion is entirely appropriate and any surgeon worth their registration will support patients in doing so. Dr Roth sees patients for second opinions regularly, and approaching these consultations with patience and without pressure is a priority. No patient should feel obliged to proceed with any surgeon they do not feel confident in.
The Difficulty of the Waiting Period
One of the most challenging aspects of revision rhinoplasty — from a psychological standpoint — is timing. The advice that patients consistently receive is that they should wait twelve to eighteen months from their primary surgery before proceeding with revision. This advice is clinically sound: the inflammatory process from the first operation needs to fully resolve before the nose is stable enough to assess accurately, and operating too early increases surgical complexity, reduces predictability, and makes the outcome less reliable.
But twelve to eighteen months is a long time to live with a result that is causing distress. Patients who are struggling often push for earlier intervention, driven by understandable urgency. The challenge for the surgeon is to honour the patient’s distress while being honest about the clinical reasons for waiting — and to help the patient understand that proceeding prematurely is not in their interest, even when it feels like the only way forward.
During the waiting period, some patients find it helpful to:
- Speak with their GP about the emotional impact, and consider referral to a psychologist if the distress is significantly affecting daily functioning
- Limit the time spent examining the nose in mirrors or photographing it — this can amplify distress without providing useful information
- Seek a consultation with a revision rhinoplasty surgeon to understand what options exist and what the likely pathway looks like — this can reduce uncertainty and give a sense of agency, even if surgery is not yet appropriate
- Connect with others who have had similar experiences — some patients find peer support helpful, though it is important to be mindful that online forums can amplify negative sentiment and do not reflect the full range of outcomes
Concerns About Body Dysmorphic Disorder
Body dysmorphic disorder (BDD) is a condition characterised by a preoccupation with a perceived defect in appearance that is either absent or minor, and which causes significant distress or impairment. It is more prevalent in people seeking cosmetic surgery than in the general population, and it is particularly relevant in the context of rhinoplasty and revision rhinoplasty — because concerns about the nose are among the most common presentations of BDD.
This does not mean that concerns about rhinoplasty outcomes are imagined or invalid. Most people seeking revision rhinoplasty have genuine, visible concerns that would be acknowledged by any surgeon who examines them. But in a subset of patients, the distress around the nose is disproportionate to what can be observed clinically, and further surgery is unlikely to provide lasting relief. In these cases, surgery may temporarily relieve distress, but the focus tends to shift to a new concern, or the previous concern returns.
Responsible surgeons screen for this. If Dr Roth has concerns that a patient’s distress around their nose may be disproportionate to the clinical findings, he will say so honestly and directly — and may recommend psychological assessment before any surgical plan is discussed. This is not a dismissal of the patient’s concerns; it is an acknowledgement that surgery is not always the right answer, and that proceeding with surgery in the presence of unrecognised BDD can cause harm. Patients who receive this feedback may find it confronting, but it is offered with the patient’s long-term wellbeing in mind.
Managing Expectations for Revision Surgery
One of the most important conversations in a revision rhinoplasty consultation is about what surgery can and cannot achieve. This conversation is more difficult — and more important — than the equivalent conversation before primary rhinoplasty, for several reasons.
First, revision rhinoplasty outcomes are genuinely less predictable than primary rhinoplasty outcomes. The altered anatomy, the presence of scar tissue, the reduced blood supply to previously operated tissues, and the unpredictability of the soft tissue response all conspire to make the result harder to forecast. A surgeon can describe what they plan to do and what they hope to achieve, but they cannot guarantee the outcome in the way that a patient who has already been disappointed once needs them to.
Second, patients who have already had a disappointing experience often arrive at revision consultation with a very precise idea of what they want changed — sometimes down to measurements and millimetres. This precision is understandable, but it can be a source of difficulty. The surgeon’s ability to achieve specific dimensional outcomes is limited by anatomy, healing, and the behaviour of grafted cartilage over time. The more specific and inflexible the patient’s expectations, the more likely that even a technically excellent revision will be perceived as inadequate.
Third, each revision procedure makes subsequent surgery more difficult. The more times the nose has been operated on, the more disrupted the tissue planes, the more depleted the cartilage sources, and the more restricted the blood supply. There is a real point at which further surgery carries greater risk of harm than benefit. Being honest with patients about where that point lies — even when it is not what they want to hear — is one of the most important responsibilities in revision rhinoplasty practice.
The goal of revision rhinoplasty is meaningful improvement — a nose that functions better, looks more like the patient hoped, and allows them to move forward. It is not perfection. Patients who can genuinely accept this framing, and who have realistic expectations of the process, tend to have the most positive experiences of revision rhinoplasty regardless of the technical outcome.
Why Revision Rhinoplasty Is Surgically More Complex
Beyond the emotional weight, revision rhinoplasty presents a distinct set of technical challenges that make it considerably more demanding than primary surgery — even for experienced rhinoplasty surgeons.
Altered Anatomy and Disrupted Planes
The tissue planes that a surgeon uses to navigate the nose during primary rhinoplasty — the clean, predictable layers between skin, subcutaneous tissue, perichondrium, and cartilage — are distorted by previous surgery. Scar tissue does not respect anatomical boundaries. Dissection in previously operated tissue requires greater care, takes more time, carries a higher risk of inadvertent injury to important structures, and produces more post-operative swelling and inflammation than the equivalent dissection in a virgin nose.
Depleted or Absent Structural Support
Primary rhinoplasty — particularly older or more aggressive techniques — often involved the removal of substantial amounts of cartilage and bone. Tip cartilages may have been over-resected, leaving the tip unsupported and liable to collapse or pinch. The dorsal septum may have been removed, destabilising the middle vault. Nasal bones may have been narrowed excessively. Each of these changes must be understood and addressed, typically by rebuilding structure using cartilage grafts from other sites.
The Soft Tissue Response
The soft tissue envelope — the skin and subcutaneous tissue overlying the nasal skeleton — responds more aggressively to a second operation than to the first. The inflammatory response is amplified. More scar tissue is produced. The skin is less able to contract smoothly over a rebuilt framework. In some patients, the soft tissue response after revision rhinoplasty is so pronounced that it obscures even technically excellent structural work beneath it. This risk is unpredictable and cannot be identified pre-operatively — it is one of the reasons revision rhinoplasty outcomes are inherently less reliable than primary outcomes.
Each subsequent revision makes this problem worse. There is a point at which the scar tissue burden becomes the dominant factor limiting what surgery can achieve, regardless of how well the structural reconstruction is executed.
Operating Time
Revision rhinoplasty consistently takes longer than primary rhinoplasty. Straightforward revision cases — where the change required is modest and the anatomy is not severely disrupted — may take three to four hours. Complex reconstruction, particularly where rib cartilage is required and multiple structural problems need to be addressed simultaneously, can take six to seven hours or more. The length of surgery cannot always be accurately estimated in advance; what appears modest in the planning may prove more involved once the anatomy is visualised directly.
Common Reasons for Seeking Revision
Patients present for revision rhinoplasty assessment with a wide range of concerns. Understanding which category a concern falls into helps clarify both the urgency and the appropriate approach.
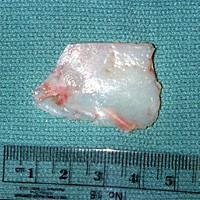
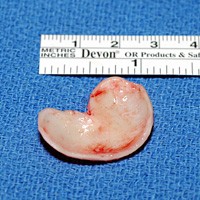
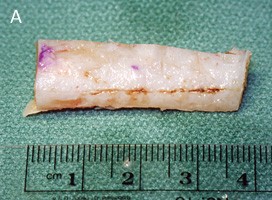
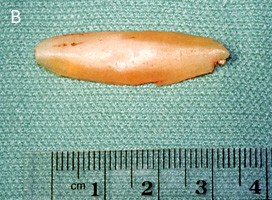
Cartilage Grafting in Revision Rhinoplasty
Almost all revision rhinoplasties require cartilage grafts to restore structural support and form. The choice of graft source depends on what is available, what the procedure requires, and what was done in the primary surgery.
The choice of graft source is not always known before surgery. Once the nasal skeleton is fully visualised under direct vision, it becomes clearer what structural elements need to be replaced or supported, and which graft materials are available and appropriate. Dr Roth will discuss the likely approach at your pre-operative consultation, with the understanding that intra-operative findings may require the plan to be adapted.
Key Clinical Considerations
Recovery After Revision Rhinoplasty
Recovery from revision rhinoplasty follows a similar structure to primary rhinoplasty recovery but is typically longer and more variable, reflecting the greater complexity of the surgery and the amplified soft tissue response.
Dr Roth’s Approach to Revision Rhinoplasty
Revision rhinoplasty requires a different mindset from primary rhinoplasty — more conservative, more cautious, and more focused on avoiding harm than on achieving a dramatic transformation. The goals are realistic improvement, not perfection; structural stability, not idealised geometry; and an outcome that allows the patient to move forward, not one that simply sets the scene for a third or fourth operation.
Dr Roth approaches every revision rhinoplasty consultation with the understanding that the patient has already had a difficult experience. The consultation is an opportunity to listen without rushing, to examine the nose carefully, to be honest about what can and cannot be achieved, and to give the patient the information they need to make a decision that is genuinely right for them — which may or may not be further surgery. Not every patient who attends a revision consultation is ultimately a surgical candidate, and saying so clearly is one of the most important things a surgeon can do.
For patients who do proceed, Dr Roth invests significant time in planning — reviewing operative notes where available, assessing what cartilage sources remain, considering what the soft tissue is likely to tolerate, and setting an honest pre-operative expectation of what the surgery can achieve. The surgery itself is meticulous and unhurried. Cartilage grafting, precise structural reconstruction, and careful soft tissue management are the technical foundations. Patience and conservatism are the governing principles.
Nearly all patients with an unsatisfactory primary rhinoplasty can be meaningfully improved with revision surgery when it is appropriately planned and timed. Absolute perfection is not achievable and is not the goal. The goal is a nose that looks better, functions better, and allows the patient to stop thinking about it.
Frequently Asked Questions
How long should I wait before seeking revision?
As a general principle, waiting 12–18 months from the primary surgery is advisable before proceeding with revision. However, seeking a consultation earlier — to understand the options and start the planning process — is entirely reasonable. A consultation does not commit you to proceeding. It gives you information, perspective, and a realistic sense of what revision can offer, which can itself be helpful during the waiting period.
Should I go back to my original surgeon?
If the relationship with your original surgeon is intact and you feel able to communicate openly with them, returning to them first is generally the right approach. They know exactly what was done and are best placed to assess what has and hasn’t worked. If you feel that relationship has broken down, or if you simply want an independent perspective, a second opinion is entirely appropriate and any responsible surgeon will support you in seeking one.
How many revision rhinoplasties can be done?
There is no fixed number, but the risk-benefit calculation changes with each successive procedure. Each revision disrupts tissue planes further, depletes cartilage sources, reduces blood supply, and increases the scar tissue burden. There is a point — which varies between individuals — at which further surgery is more likely to cause harm than to achieve improvement. An honest surgeon will tell you if they believe you have reached that point.
Will revision rhinoplasty fix my breathing as well?
It may, depending on the cause. Nasal valve collapse — one of the most common functional complications of rhinoplasty — can often be addressed with alar batten or lateral crural strut grafts as part of revision surgery. A deviated septum, if it was not adequately corrected in the primary procedure, can be addressed concurrently. The specific causes of any breathing difficulty are assessed at consultation.
I am finding the waiting period very difficult. What can I do?
This is one of the most common and understandable challenges in revision rhinoplasty. Speaking with your GP about the distress you are experiencing is a good first step — they can provide support directly and, if appropriate, refer you to a psychologist or counsellor. Booking a consultation with a revision rhinoplasty surgeon to understand your options can also help reduce the uncertainty that makes waiting harder. The knowledge that there is a plan — even if surgery is still months away — is often genuinely helpful.
Contact us to arrange a consultation → | Rhinoplasty Surgery → | Recovery — Month by Month → | Rhinoplasty Risks → | Allograft vs Own Rib → | Rib Grafts →
View Rhinoplasty Before & After Gallery →
Specialist Otolaryngologist & Head and Neck Surgeon
Specialist registration — Otorhinolaryngology, Head & Neck Surgery
View full profile