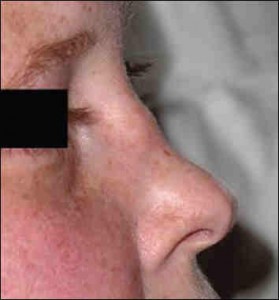
Saddle Nose Correction
All cosmetic surgery involves risks and individual results vary. Cosmetic surgery is a serious decision. Decisions about whether to proceed should be made after careful consideration and following at least two consultations with a qualified medical practitioner.
A saddle nose deformity refers to a collapse of the nasal bridge that produces a concave or depressed dorsal profile — the nose appears to dip in the middle rather than forming a straight or gently curved line from the brow to the tip. The name reflects the shape of the resulting profile. Saddle nose deformity can range from a subtle softening of the dorsal line to a severe structural collapse with significant functional and cosmetic consequences. Correction requires reconstruction of the nasal framework using cartilage grafts, and the extent of reconstruction required depends on the severity of the collapse and the condition of the remaining supporting structures.
All surgery carries risks — read the full rhinoplasty risks page →
Causes
Saddle nose deformity results from loss of structural support in the nasal dorsum — most commonly from damage to or loss of the cartilaginous or bony framework that maintains the height of the bridge.
Nasal trauma is one of the most common causes. A fracture that disrupts blood supply to the septal cartilage — or that causes a septal haematoma that goes untreated — can result in avascular necrosis of the cartilage, which collapses over time. The consequence may not be apparent immediately after the injury and can develop months to years later.
Previous surgery is a frequent cause of iatrogenic saddle nose deformity. Rhinoplasty or septoplasty that removed too much cartilage from the dorsum or the L-strut of the septum — leaving insufficient structural support — can result in progressive collapse of the bridge. The deformity may develop gradually as residual cartilage weakens under the mechanical forces of breathing and overlying soft tissue.
Granulomatosis with polyangiitis (GPA) — previously called Wegener’s granulomatosis — is an autoimmune condition that causes inflammation and destruction of cartilage and bone, including in the nose and sinuses. Saddle nose deformity is a recognised feature of GPA and can develop progressively as the condition erodes the nasal framework. Surgical correction in active GPA requires disease control first.
Cocaine use is a well-recognised cause of progressive nasal septal destruction. Regular intranasal cocaine use causes vasoconstriction of the blood vessels supplying the septal mucosa, leading to ischaemia, ulceration, and eventual cartilage and bone destruction. The resulting defect can be extensive and involves both the septum and the nasal bridge.
Relapsing polychondritis and other conditions affecting cartilage can also cause saddle nose deformity, as can syphilis — historically a common cause, now rare.
Functional Consequences
Saddle nose deformity is not purely a cosmetic problem. The structural collapse that produces the visible deformity also narrows or obstructs the nasal airway, compresses the internal nasal valve, and may destabilise the nasal tip. Many patients with significant saddle deformity have impaired nasal breathing as well as cosmetic concerns, and both should be assessed and addressed in the surgical plan.
Surgical Correction
Correction of saddle nose deformity is performed through an open rhinoplasty approach, which provides direct access to the dorsum and the septal framework. The surgical plan depends on the degree of collapse and the condition of the remaining structures.
For mild saddle deformities with intact septal support, augmentation of the dorsum using septal or ear cartilage grafts may be sufficient. A dorsal onlay graft — placed over the existing dorsum to restore height — is the standard approach for limited deformities.
For moderate to severe deformities, where the L-strut of the septum has been lost or significantly compromised, reconstruction requires rebuilding the structural framework of the nose from the inside out. This typically involves placement of a new septal support structure — either reconstructed from the patient’s own cartilage or from a rib cartilage graft — before the dorsal augmentation is placed. Without restoring the internal framework first, an onlay graft alone will not produce a stable long-term result.
Rib Cartilage for Saddle Nose Reconstruction
Most significant saddle nose deformities require rib cartilage as the graft source, because the volume of cartilage needed exceeds what the septum or ear can reliably provide — particularly in revision cases where septal cartilage has already been used or removed.
Dr Roth’s preference for large saddle nose reconstructions is irradiated cadaveric rib cartilage allograft rather than the patient’s own (autologous) rib. Irradiated cadaveric rib has been shown to have a low warping rate compared with fresh autologous rib, avoids the donor site morbidity associated with harvesting the patient’s own rib cartilage (chest wall pain, scar, and the small risk of pneumothorax), and provides an adequate and predictable volume of straight graft material. The irradiation process sterilises the graft and eliminates the risk of disease transmission. In cases where autologous rib is preferred — or where allograft is not available or appropriate — the patient’s own rib can be harvested instead. This is discussed at consultation based on the individual case.
Read more about allograft versus own rib cartilage →
Dr Roth’s Clinical Perspective
Saddle nose reconstruction is one of the more technically demanding rhinoplasty procedures because the structural problem is internal — the framework that everything else depends on has been lost — and rebuilding it requires restoring support from the ground up before addressing the external appearance. An onlay graft placed on an inadequately supported dorsum will not hold its position long term. The internal reconstruction has to come first.
My preference for irradiated cadaveric rib in significant cases reflects the practical reality that warping is the main complication of rib grafts in rhinoplasty, and irradiated allograft warps less predictably than fresh autologous rib. It also avoids putting the patient through a chest harvest, which adds meaningful pain and recovery time to an already significant procedure. The outcomes with irradiated allograft in my hands have been reliable, and I explain the graft choice in detail at consultation so patients understand what material is being used and why.
Most patients presenting with saddle nose have had a previous rhinoplasty or septoplasty, or have a history of nasal trauma. The consultation therefore involves a careful review of what was done previously, what cartilage remains, and what the realistic goals of reconstruction are. This is not a procedure where expectations should be set casually — the aim is meaningful structural and functional improvement, not perfection, and patients who understand that going in have better outcomes.
— Dr Jason Roth, MBBS, FRACS (ORL-HNS), IBCFPRS
Revision Rhinoplasty → | Allograft vs Own Rib → | Rhinoplasty Risks → | Contact Us →
Specialist Otolaryngologist & Head and Neck Surgeon
Specialist registration — Otorhinolaryngology, Head & Neck Surgery
View full profile | Revision Rhinoplasty →